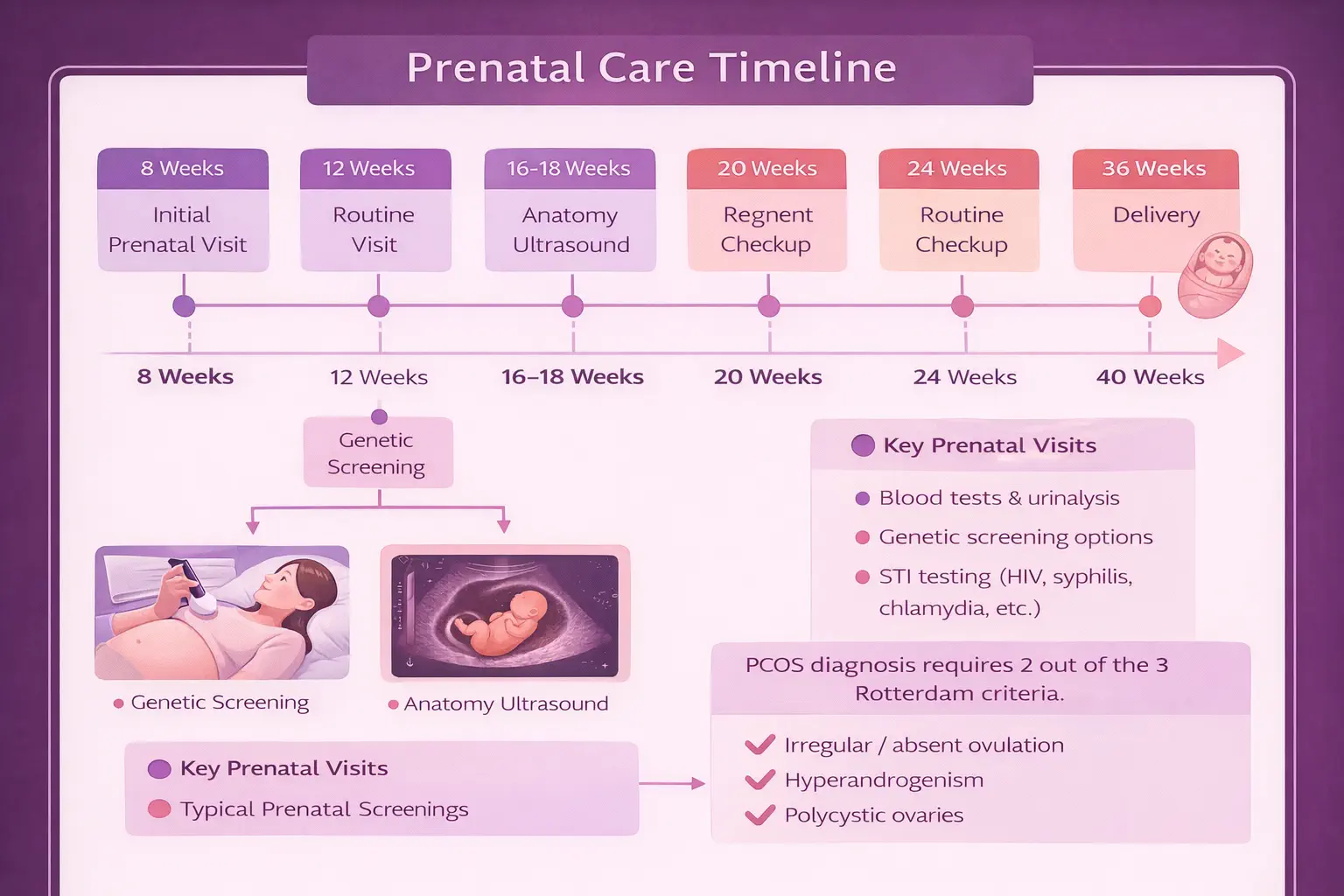
The third trimester is when prenatal visits increase in frequency and the focus
shifts toward delivery preparation. Your baby is gaining weight, lungs are maturing,
and the body is preparing for labor. Monitoring becomes more intensive because most
pregnancy complications — preeclampsia, gestational diabetes-related issues,
growth problems — either emerge or intensify during this period.
More Frequent Visits
Beginning at 28 weeks, visits shift to every 2 weeks, and at 36 weeks, to weekly.
Each visit includes routine vital signs, fundal height measurement, fetal heart tones,
and urine dipstick. The increasing frequency ensures that changes in blood pressure,
fetal growth, or other parameters are caught early.
Group B Streptococcus Screening (36–37 Weeks)
Group B Strep (GBS) is a bacterium that is carried in the vaginal or
rectal area in approximately 25 percent of women. While harmless to the mother, GBS
can be transmitted to the newborn during delivery and cause serious neonatal infection.
A vaginal and rectal swab is performed at 36 to 37 weeks. If the
culture is positive, you receive intravenous antibiotics during labor
to significantly reduce the risk of neonatal transmission.
Fetal Position Assessment
As your due date approaches, fetal position becomes clinically relevant. Most babies
settle into a head-down (vertex) position by 36 to 37 weeks. If the baby is breech
(bottom or feet down), Dr. Broad discusses options including external cephalic
version (ECV) — a manual procedure to encourage the baby to turn — and
the timing and mode of delivery.
Cervical Checks
Cervical exams in the third trimester are performed when clinically
appropriate — not automatically at every visit. They assess cervical
dilation, effacement, and fetal station. While useful for evaluating readiness when
specific symptoms or timing warrant it, cervical dilation alone is not a reliable
predictor of when labor will begin.
Birth Plan Discussion
In the third trimester, Dr. Broad discusses your preferences for labor and
delivery, including pain management options (epidural, IV medications, non-pharmacologic
approaches), laboring positions, immediate skin-to-skin contact, delayed cord clamping,
and breastfeeding initiation. A birth plan is a communication tool — it helps
your care team understand your priorities while acknowledging that flexibility may be
needed depending on how labor progresses.
Labor Signs Education
Understanding the difference between true labor and false labor (Braxton Hicks
contractions) is essential. Third trimester visits include education on when to go
to the hospital: regular contractions that increase in frequency and intensity,
rupture of membranes (water breaking), significant vaginal bleeding, or decreased
fetal movement.
Cord Blood Banking
Cord blood contains hematopoietic stem cells that can be used to treat certain blood
disorders and cancers. If you are interested in cord blood banking — either
private or public donation — the third trimester is the time to discuss this
and make arrangements. Dr. Broad provides information on both options so you
can make an informed decision.
High-Risk Patients: Additional Monitoring
Women who have developed high-risk conditions during pregnancy — gestational
diabetes requiring medication, preeclampsia concerns, fetal growth restriction, or
other complications — may begin additional monitoring in the third trimester,
including the non-stress test (NST) and biophysical profiles
(BPP). For details on what this monitoring involves and what the results
mean, see the high-risk pregnancy
care guide.