There are five FDA-approved intrauterine devices available in the United States, and the best
choice depends on your health goals, bleeding preferences, and how long you want protection.
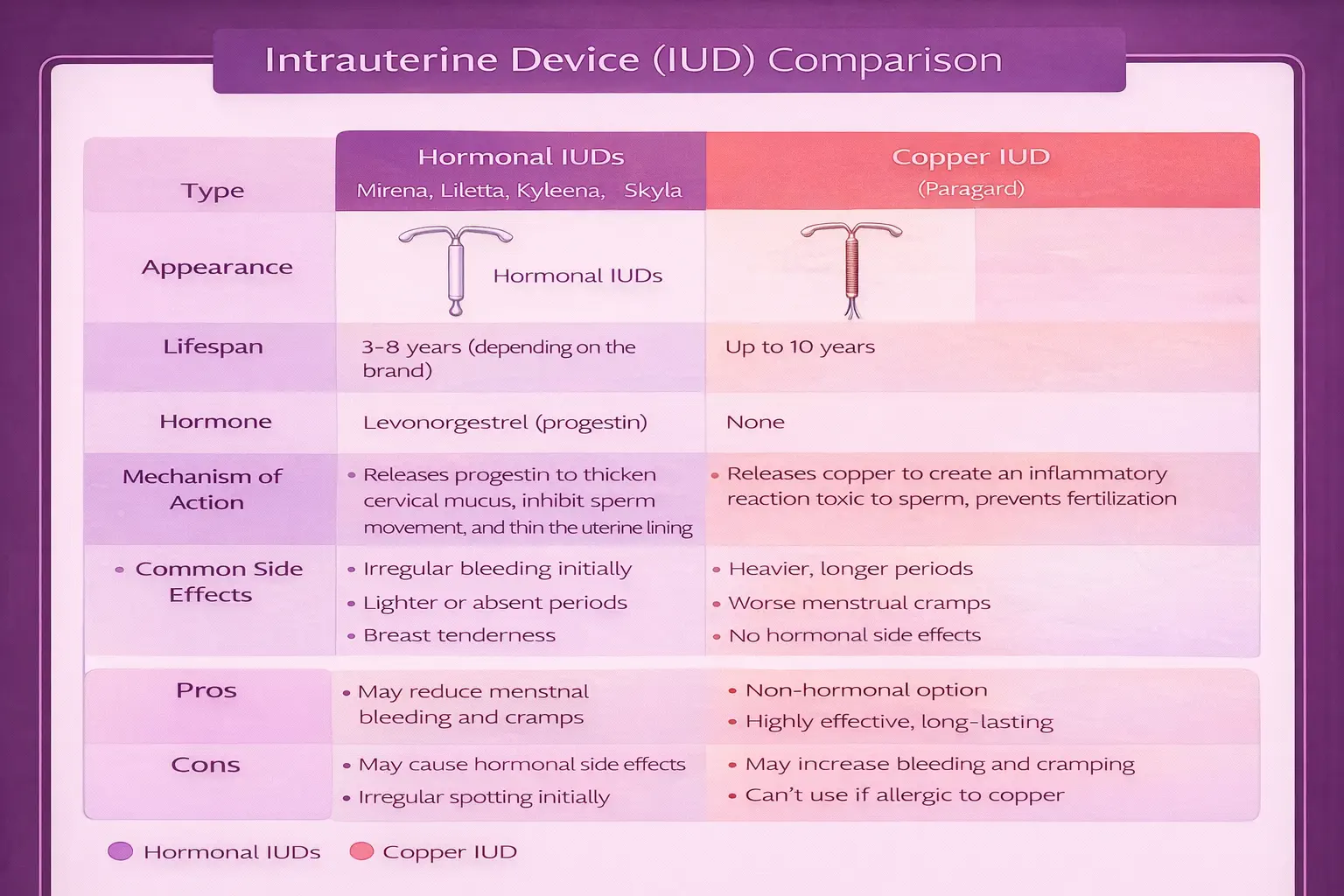
The four hormonal IUDs release levonorgestrel (a progestin) locally within
the uterus, which thins the uterine lining and thickens cervical mucus. The one
non-hormonal IUD uses copper to create an environment that is toxic to sperm.
Hormonal IUDs
Mirena contains 52 mg of levonorgestrel and is FDA-approved for up to
8 years of contraception. It is also FDA-approved for the treatment of
heavy menstrual bleeding (menorrhagia), making it a dual-purpose device.
Most women experience significantly lighter periods, and approximately 20% stop having
periods altogether by one year. Mirena is the most widely studied IUD in the world.
Kyleena contains 19.5 mg of levonorgestrel and is approved for up to
5 years. Its lower hormone dose and smaller frame make it
a popular choice for women who want hormonal contraception with fewer systemic effects.
Periods typically become lighter but are less likely to stop completely compared to Mirena.
Liletta contains 52 mg of levonorgestrel — the same dose as Mirena —
and is approved for up to 8 years. It was developed through a public-private
partnership to improve IUD access and is often available at lower cost through public health
programs and Title X clinics.
Skyla contains 13.5 mg of levonorgestrel, the lowest dose of any hormonal IUD,
and is approved for up to 3 years. It has the smallest frame
of all IUDs and the narrowest insertion tube, which may be preferred by nulliparous women
or those with a smaller uterine cavity.
Non-Hormonal IUD
Paragard is the only hormone-free IUD available in the United States. It is
wrapped in copper wire, which creates a local inflammatory response that is toxic to sperm
and prevents fertilization. Paragard is approved for up to 10 years and is
the right choice for women who want long-term, hormone-free contraception.
It can also be used as emergency contraception if inserted within 5 days of
unprotected intercourse — the most effective form of emergency contraception available.
The trade-off: Paragard may increase menstrual bleeding and cramping, particularly in the
first 3–6 months. This typically improves over time, but women with already-heavy periods
may prefer a hormonal IUD instead.
ACOG recommends long-acting reversible contraceptives (LARCs) — IUDs and implants
— as first-line contraceptive options for most women, including adolescents and
nulliparous women. LARCs have the highest continuation rates and lowest failure rates of all
reversible contraceptive methods.
ACOG Committee Opinion No. 642, 2015; reaffirmed 2023